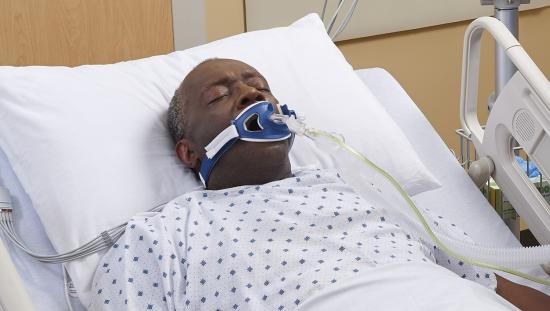
High flow oxygen therapy involves the use of warm, humidified oxygen delivered via nasal cannula (also referred to as high flow nasal cannula oxygen therapy - HFNO) under positive end expiratory pressure (PEEP).[1] High flow oxygen therapy was originally implemented for neonates, but has gained more attention in adults due to several factors.
By administering warm and humidified gas, airway dehydration is reduced, and secretion clearing is increased. There is also a higher FiO2 delivery when compared to face mask use. Plus, using PEEP allows for an increase in end-expiratory lung volume and alveolar recruitment.1
During the COVID-19 pandemic where more patients may experience acute respiratory failure, healthcare professionals and organizations have turned to high flow oxygen therapy as a way to support these patients.
In addition to clinical benefits of high flow oxygen therapy, the practical benefit of using an oxygen delivery system that does not require critical care oversight is extremely valuable in healthcare settings overwhelmed with patients needing respiratory support.1
This article discusses both the clinical and practical benefits of high flow oxygen therapy and how they’ve been successfully applied to COVID-19 patients who have acute hypoxemic respiratory failure.
Patient Comfort Increases with High Flow Oxygen Therapy2
It’s been well established that face masks with a reservoir bag, while a first line therapy, provide little when it comes to patient comfort. The air is dry, and the masks prevent patients from doing many basic functions.
Wearing a face mask hinders the patient from communicating, drinking, or eating without removing the mask. Face masks can also cause patient distress and increase the risk of skin breakdown.2
High flow oxygen therapy mitigates both of these concerns. Firstly, the air is warmed and humidified, reducing the drying effects of oxygen therapy.2 This also reduces the risk of airway dehydration, which can lead to pain and discomfort, epistaxis, and other pulmonary issues.
Alternatively, high flow oxygen therapy is administered via nasal cannula rather than a face mask. This frees the patient’s mouth to talk, drink, and eat while benefiting from oxygen therapy.2 And while the risk for skin breakdown still exists with a cannula, there is less surface area contacting the patient during oxygen administration.
High Flow O2 Therapy Provides Noninvasive Benefit to Patients with Severe COVID-19 Related HRF
Using humidified high flow nasal oxygen is useful in patients with severe COVID-19 related hypoxemic respiratory failure (HRF) as a noninvasive intervention.2
Patients using high flow oxygen may be able to be safely weaned without the need of mechanical ventilation.[2] Using noninvasive respiratory support in patients with COVID-19-related respiratory failure has been critical in areas that lack proper respiratory support. This may be due to lack of physical resources (ventilators or oxygen) or due to a lack of healthcare personnel available.
In a study exploring the use of high flow oxygen for patients with COVID-19 in hospitals lacking sufficient respiratory resources, nearly half (47%) of patients treated with high flow oxygen therapy were considered successful. These patients did not require invasive maneuvers including intubation. Patients utilized high flow oxygen therapy for an average of six days.2 This study also notes 93% of those successful patients were safely discharged from the hospital.2
High Flow O2 Therapy Provides Interventions Obtainable Outside the ICU Setting
A major challenge for healthcare providers and organizations caring for patients with COVID-19 is access to beds and rooms. ICUs and step-down units were often beyond capacity, highlighting the need for interventions that can be done safely outside of an ICU setting.
High flow oxygen therapy has proven to be one of these vital interventions that can be done in a non-critical care setting. This alone increases the volume of COVID-19 patients in which a hospital or institution can support where they may experience hypoxemic respiratory failure.3
Furthermore, high flow oxygen therapy is a type of respiratory support that does not require advanced training to implement and monitor. This allows healthcare workers outside of critical care settings to safely administer and monitor patients using high flow O2.4
High Flow O2 Therapy May Reduce Intubation Rates in Patients with COVID-195
The use of high flow oxygen therapy (HFNO) has been evaluated in several studies specifically focused on patients with COVID-19. A retrospective study out of France found patients who undergo HFNO were less likely to need mechanical ventilation (56% of HFNO group versus 71% in non-HFNO group).5 The mortality rate of these patients with COVID-19 respiratory failure was reduced when they received HFNO.6
These studies found high flow oxygen therapy to be a safe and effective intervention in patients with COVID-19 related respiratory failure and works well as a way to avoid escalation. HFNO was also shown to both improve overall oxygenation and reduce pneumonia in these patients.6
Most of these studies with COVID-19 patients are considered small to medium size (ranging for 100-379 patient sample sizes), but the congruent outcomes of these trials show the benefit and efficacy of implementing HFNO in patients with acute respiratory failure due to COIVD-19 infections.6
But when looking at high flow oxygen therapy versus conventional oxygen in general (as opposed to COVID-19 patients specifically) a systematic review and meta-analysis of nine trials and over 2,000 patients found no difference in mortality.6 This review further supports that high flow oxygen therapy is safe and effective when it comes to noninvasive respiratory support in patients with acute hypoxemic respiratory failure.
Additional Benefits of High Flow Oxygen Therapy
High flow O2 therapy is not only a practical intervention for patients with COVID-19 related hypoxemic respiratory failure, but it also provides additional physiological benefits. These benefits include: 2
- Alveolar recruitment
- Improved perfusion matching
- Reducing airway resistance
- Reduced respiratory effort
- Decreased oxygen dilution
- Decreased dead space
- High levels of humidification
While more studies are needed to explore the use of high flow oxygen therapy in patients with COVID-19 specifically, there is clearly a benefit of using this treatment in these patients. Patient comfort is increased, it is noninvasive and can be done outside of a critical care setting, all while being a very effective and successful way to support certain patients from a respiratory standpoint.
As with all interventions, careful monitoring of respiratory parameters is required to maintain patient safety and implement additional measures as quickly as possible.
References
- Ashraf-Kashani, N et al. (2017) High-flow nasal oxygen therapy. BJA Education, 17 (2):57–62.
- Calligaro G. et al. (2020) The utility of high-flow nasal oxygen for severe COVID-19 pneumonia in a resource-constrained setting: a multi-center prospective observational study. E Clinical Medicine 28:100570.
- Lyons, C & Callaghan, M. (2020). The use of high-flow nasal oxygen in COVID-19. Anaesthesia. 75(7): 843-847.
- Jackson, J et al (2021). Implementation of high-flow nasal cannula therapy outside the intensive care setting. Respiratory Care. 66(3): 357-365.
- Demoule, A et al. (2020). High-flow nasal cannula in critically iii patients with severe COVID-19. American journal of respiratory and critical care medicine.202(7):1039-1042.
- Rochwerg, B. et al. (2019). High flow nasal cannula compared with conventional oxygen therapy for acute hypoxemic respiratory failure: a systematic review and meta-analysis. Intensive Care Med. 45:563-572.
© GE, 2021 – All rights reserved.
GE and the GE Monogram are trademarks of GE. Reproduction in any form is forbidden without prior written permission from GE. Nothing in this material should be used to diagnose or treat any disease or condition. Readers must consult a healthcare professional.
JB17743XX