What is neuromuscular transmission?
Neuromuscular transmission (NMT) is the transfer of an impulse between a nerve and a muscle in the neuromuscular junction. NMT can be blocked by neuromuscular blocking agents – drugs which cause transient muscle relaxation and prevent the patient from moving and breathing spontaneously.
Muscle relaxation is used during general anesthesia to enable endotracheal intubation and to provide the surgeon with optimal working conditions. In critical care, muscle relaxation is used during mechanical ventilation to minimize the patient’s work of breathing and to improve oxygenation.
How is the NMT block measured?
The level of neuromuscular block is routinely measured by stimulating a peripheral nerve, usually in the hand and by subjectively evaluating the muscle response either visually or tactilely with a device. Evidence suggests that subjective neuromuscular monitoring techniques can’t determine adequate recovery from neuromuscular blockade and as a consequence, a large percentage of patients arrive to the PACU with residual paralysis.1
By comparison, GE HealthCare offers the NMT module, which provides quantitative, automatic measurements of muscle response to stimulus and consequentially, the level of block. This objective measurement can be used to assess the adequate level of blockade throughout the surgery and safely time the administration of antagonist and extubation to help avoid occurrence of residual paralysis.
NMT sensor types
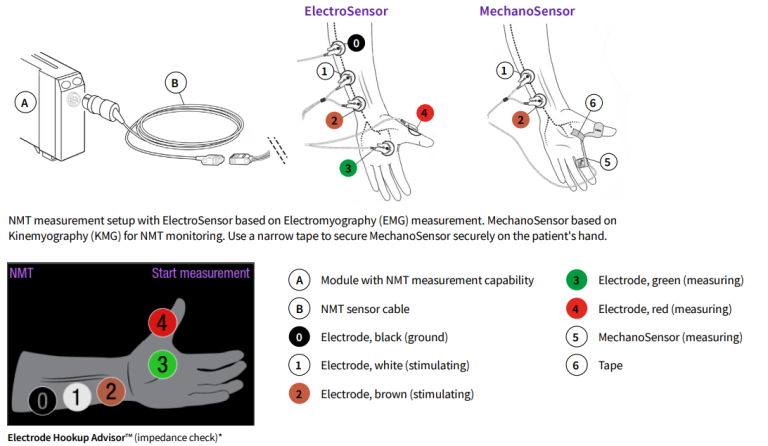
GE HealthCare offers two different sensor types for the NMT module.
- The re-usable ElectroSensor™ can be used on the patient's hand or foot in both adult and pediatric patients. They work reliably even when the hand movement is obstructed. The ElectroSensor directly measures the electrical activity of the muscle with recording electrodes, quantifying the response to nerve stimulation.
- The MechanoSensor™ measures the motion of the thumb with a piezoelectric sensor, which converts the physical motion to an electrical signal and quantifies the evoked mechanical response. The MechanoSensor sensor is available in adult and pediatric sizes.
Adequacy of Anesthesia
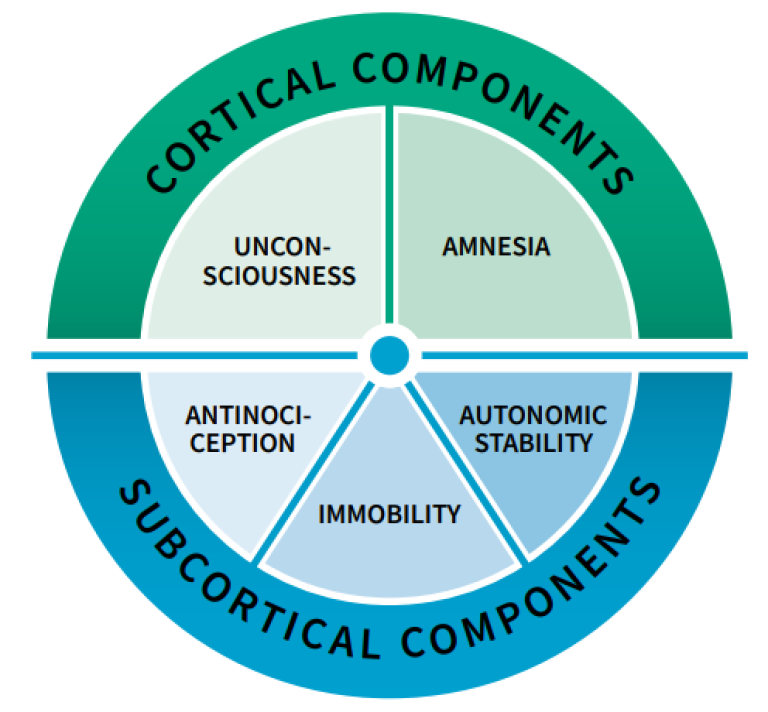
Adequacy of Anesthesia consists of several interrelated components as depicted below.
One of the objectives of general anesthesia is immobility, i.e., the assurance that the patient does not move. Often neuromuscular blocking agents are used to achieve this goal. Anesthetic agents prolong and amplify the effects of neuromuscular blocking agents, therefore, it is recommended to use quantitative NMT monitoring when anesthetic agents are used together with neuromuscular blockade. NMT is an important part of adequacy of anesthesia concept and, when combined with other parameters such as the Entropy and hemodynamic measurements, it helps to achieve a more complete picture of the patient’s status.
Nerve stimulus
A supramaximal stimulus is recommended to ensure that all muscle fibers are stimulated with sufficient intensity and that reliable measurements are achieved during deep neuromuscular block. The NMT module automatically determines the current needed for the supramaximal stimulus and maintains this current throughout the procedure.
Train-of-four (TOF) is used as the default stimulation mode. Four supramaximal stimuli are generated at 0.5 second intervals. In an unrelaxed patient, each stimulus in the train causes the muscle to contract.
Stimulation modes
- Train of four, TOF: Recommended for most cases. It is also the default setting.
- Double burst stimulation, DBS: It enables better visual observation of the fading in responses.
- Post tetanic count, PTC: Used for estimating the relaxation level with tetanic stimulation.
- Single twitch, ST: Single twitch mode is practical when using depolarizing relaxants: in this case, TOF% does not give any additional information about the patient status.
Quantitative muscle response
The muscle response can be quantified with different parameters depending on the type and the level of neuromuscular block.
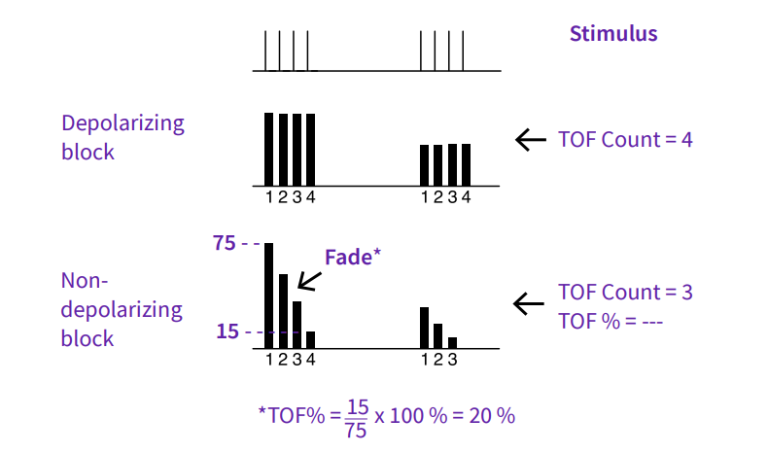
TOF Count is the number of detected muscle responses. Train- of-four ratio (TOF%) is the ratio of the fourth muscle response to the first one. TOF% indicates fade in non-depolarizing block. Once the TOF Count drops below four responses or T1% is less than 10%, the TOF% is not calculated.
When depolarizing agents are used, no fade occurs, and the height of the four responses indicates the level of block.2

When no responses are detected to TOF stimulation, the post tetanic count (PTC) is the only way to measure the neuromuscular block. A tetanic stimulation (50 Hz) is generated for five seconds and post-tetanic responses to single twitch stimulation are counted. The larger the PTC, i.e., the number of detected responses, the sooner the normal TOF responses return.2
Monitoring of neuromuscular block in five steps
- Properly secure the sensor of choice (as depicted on page 1). Press measurement start-up. Monitor will start the measurement by setting the stimulus current automatically and by performing a reference measurement. With the unrelaxed patient, TOF% is 100.
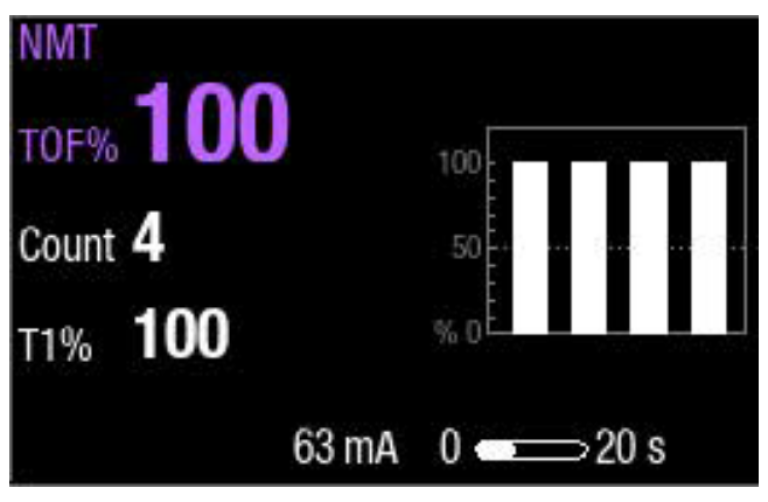
2. Non-depolarizing relaxants cause a fade in the responses, indicated by a lower TOF% and a slope in the bar graph. Depolarizing relaxants result in an equal drop in all four responses, without fade.
3. Neuromuscular block can be used to facilitate endotracheal intubation. The physician can use the time when all responses disappear (i.e., TOF Count is 0) as a guide to determine when to intubate.
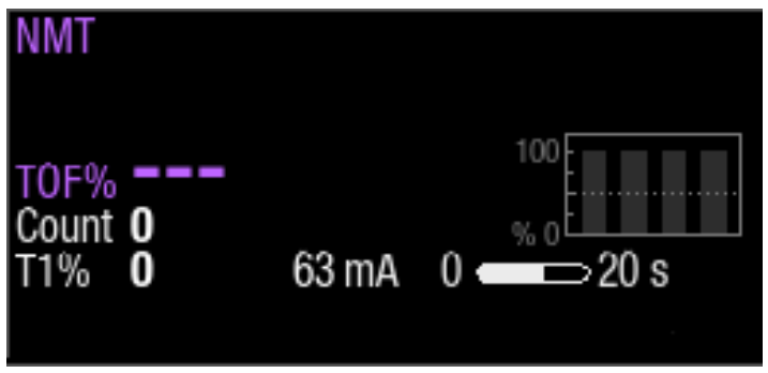
4. During surgery and in critical care, TOF Count is used to maintain steady optimal level of neuromuscular block. When TOF Count exceeds a level set by the user, the GE HealthCare monitor will give a “Block recovery” message

5. Based on type of reversal agent you want to use; you can time the administration by using TOF % and twitch count. For safe extubation, TOF% should be higher than 903 .
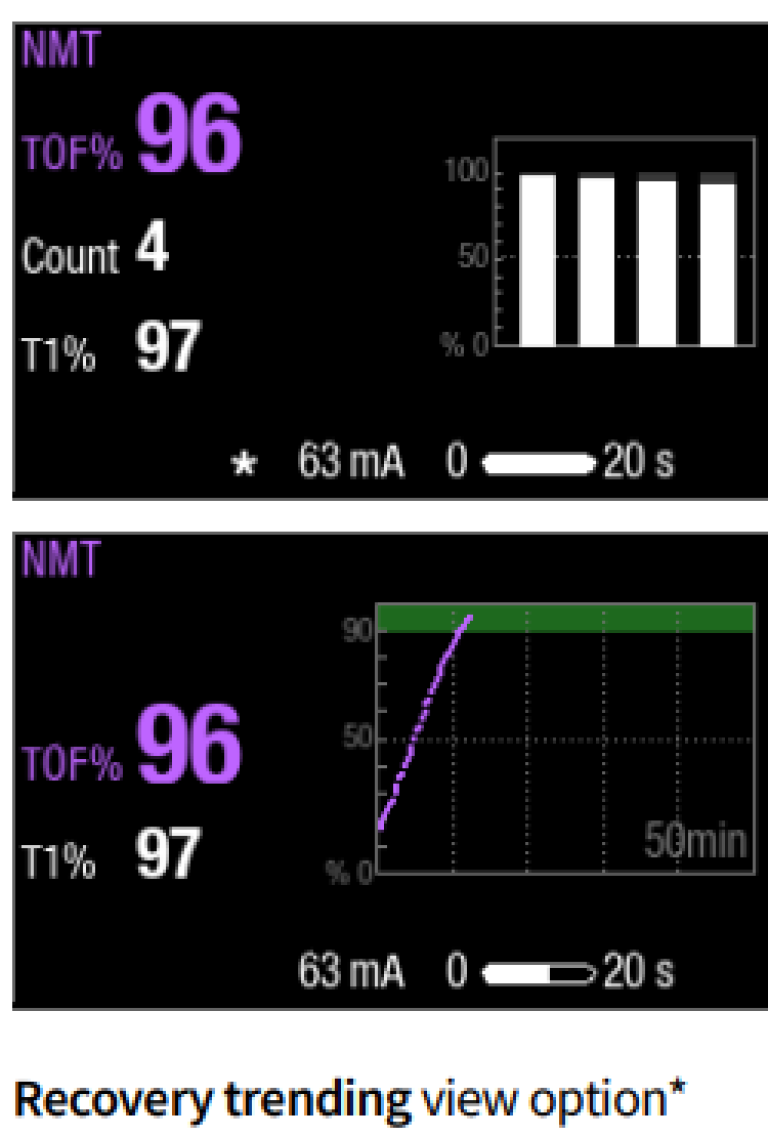
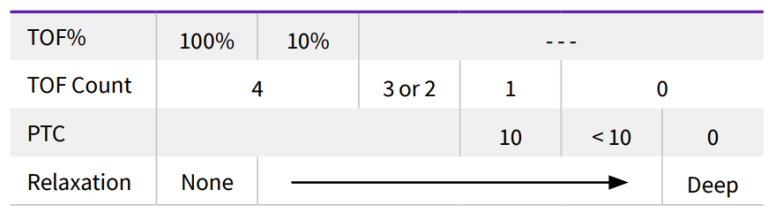
How to interpret the NMT values
When neuromuscular block deepens, different stimulation modes may be needed to assess the relaxation status. The following table describes the depth of relaxation4 .
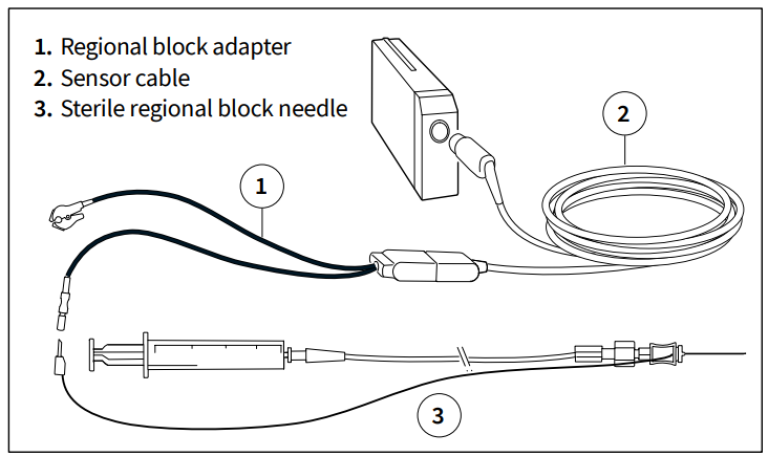
Nerve location for regional block
The NMT module can also be used to locate the nerve to be blocked in regional anesthesia.
A regional block needle is stimulated with small, repeated 2.0 mA stimuli while the nerve is approached. Each nerve stimulus should result in muscle contraction. The closer the needle is to the motor nerve, the lower the current is needed to give a response. When even a small stimulus current (e.g., < 0.5mA) results in a visible muscle contraction, the optimum site has been located and local anesthetic can be injected.
This method helps clinicians find the optimum site of the regional nerve to be blocked and, thus, optimizes the bolus of the anesthetic to be injected. The correct location also protects the patient against mechanical nerve and vessel lesions.
Why use the NMT module?
Automatic and hands-free
Neuromuscular block measurements with the NMT module are easy. Simply attach the sensor and push the Start-up key.
The module will set the supramaximal current and automatically cycle according to the user-defined measurement interval.
Optimal dosage during anesthesia and in critical care
Quantitative NMT monitoring gives a clear picture of the individual dosage needs of the patient and helps the clinician facilitate optimal and cost-effective administration of neuromuscular blocking drugs.
Optimized recovery
Monitoring the level of neuromuscular block enables follow-up and prediction of recovery and helps in correct timing of the antagonists, which may decrease the incidence of residual paralysis.
Enhanced patient safety
Objective, quantitative monitoring is one of the only means to safely indicate recovery of neuromuscular block (TOF%>90%).3 Therefore, utilizing the NMT module may help decrease the incidence of residual paralysis which has been associated with respiratory complications.
Fast patient throughput
Patients that arrive to the PACU with residual paralysis (TOF%<90) stay on average 90 minutes longer.5 Using NMT to guide extubation times can support shorter length of stay.
Integrated information
When the NMT measurement is integrated in a monitoring system, the measured values are displayed, trended and automatically documented together with all the other monitored parameters.
Additional resources
For white papers, guides and other instructive materials about our clinical measurements, technologies and applications, please visit http://clinicalview.gehealthcare.com/
References
- Murphy GS, Brull SJ. Residual neuromuscular block: Lessons unlearned. Part 1: Definitions, incidence, adverse psychological effects of residual neuromuscular block. Anesth Analg 2010;111:120-128
- Naguib M, Brull SJ, Johnson KB: Conceptual and technical insights into the basis of neuromuscular monitoring. Anaesthesia 2017; 72 (Suppl. 1), 16-37.
- Naguib M, Brull SJ, Kopman AF, et al. Consensus Statement on Perioperative Use of Neuromuscular Monitoring. Anesth Analg 2018; 127:71-80.
- Howardy-Hansen P, Viby-Mogensen J, Gottschau A, et al., Tactile Evaluation fo the Posttetanic count (PTC). Anesthesiology 1984, 60:372-374.
- Butterly A, Bitner EA, George E, Sandberg WS, Eikermann M, Schmidt U. Postoperative residual curarization from intermediate-acting neuromuscular blocking agents delays recovery room discharge. Br J Anaesth. 2010; 105: 304-309.