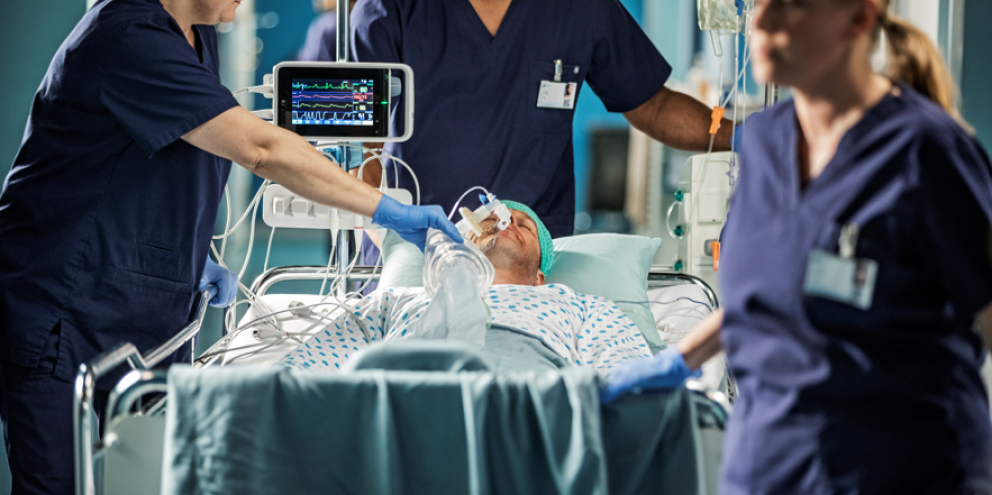
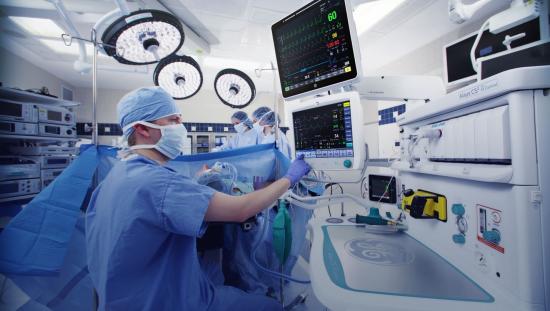
EARLY DETECTION of patient deterioration to optimize patient safety in general wards is critically important, yet VERY CHALLENGING
DETERIORATION OF PATIENTS on general wards often goes unnoticed for prolonged periods of time
In one study, nurses doing spot checks every four hours missed 90% of hypoxemic events in which saturation was <90% for at least one hour, and in another study, at least 42% of patients had been checked by the nurse within two hours of a respiratory depression event.1 Most ward patients are monitored a very small fraction of the time
ADVERSE EVENTS in general wards are not uncommon, and many are preventable
- Post-operative death accounts for 7.7% of all deaths globally, making it the third greatest contributor to deaths.2
- 73% of patients who died in-hospital were not admitted to critical care at any stage after surgery. 3
- A study of med-surg ward patients showed that those who experience a cardiac arrest have significantly different vital signs from other patients in the 48 hours prior, suggesting outcomes may be altered with earlier intervention.4
DELAYED INTERVENTION can profoundly impact patient outcomes
Evidence exists that for many conditions – sepsis for example – later or delayed intervention is associated with higher in-hospital mortality. 5,6
A study that continuously monitored pulse rate and SpO2 showed a significant decrease in RRT activations and ICU transfers. Other studies have reported a reduction in hospital length of stay and mortality when intensifying and automating ward monitoring. 7
RELYING ON MANUAL SPOT CHECKS to monitor ward patients is suboptimal and can INCREASE the risk of PATIENT DETERIORATION AND SAFETY ISSUES
Vital signs are often abnormal, or trending toward abnormal, hours before cardiac arrest or ICU transfer. But clinicians may only suddenly notice because spot-checks are usually done on a 4-6 hr interval.8
In one study, nurses recorded nearly 72% of RRs as 18 or 20 bpm, whereas only 13% measured by trained observers had these values, confirming a significant bias and/or multiplication artefact.9
Postoperative respiratory deaths are nearly all preventable. Most ward hypoxaemia and hypotension is missed because ward monitoring typically consists of vital signs assessed at intervals of 4 to 8 hours.10
EARLY IDENTIFICATION of patient deterioration to improve patient safety and outcomes REQUIRES A CONTINUOUS APPROACH to monitoring
CONTINUOUS MONITORING OF RR, IN ADDITION TO SpO2 AND PR, IS AN EFFECTIVE WAY OF RECOGNIZING PATIENT DETERIORATION EARLY
RR is viewed as “the sentinel and arguably most important vital sign because its normal values are breached before those of other vital signs in nearly all states of clinical decline.”11
Measurement of RR provides information that pulse oximetry cannot provide. The two measurements are complementary and should not be substituted for one another.12
The National Institute for Clinical Excellence recognizes RR as the most sensitive marker of a deteriorating patient and the first observation to indicate a problem.13
Abnormal RR has been shown to be an important predictor of serious events such as cardiac arrest and admission to an ICU.12
EARLY IDENTIFICATION OF DETERIORATION CAN HELP REALIZE POSITIVE IMPACTS ON OPERATIONS AND PATIENT OUTCOMES
Reduced transfers to higher acuity units Data from a study of continuous ward monitoring of SpO2 and HR showed a reduction in ICU transfer rate, which led to a significant annual cost savings.14
Reduced LoS Another study of continuous monitoring of RR and HR on a medical-surgical unit showed a significant decrease in total length of stay in the hospital and decrease in ICU days for transferred patients.15
Improved outcomes “Early identification of deterioration… enables rapid targeted management, can help reduce need for transfer to higher acuity units, reduce hospital lengths of stay and costs, and improve survival rates.”16
References:
- Sun Z, et al., Postoperative hypoxemia is common and persistent: a prospective blinded \observational study. Anesth Analg; 121: 709-15 (2015).
- Nepogodiev, et al., Global burden of postoperative death. The Lancet; Vol 393, Issue 10170, P401 (2019).
- Rupert M Pearse, et al., Mortality after surgery in Europe: a 7-day cohort study. The Lancet; 380(9847): 1059-1065 (2012).
- Churpek, et al., Predicting Cardiac Arrest on the Wards, A Nested CaseControl Study. CHEST; 141/5 (2012).
- Bates, et al., Finding patients before they crash: the next major opportunity to improve patient safety. BMJ Qual Saf (2015).
- van Zanten, et al., Guideline bundles adherence and mortality in severe sepsis and septic shock. Crit Care Med; 42:1890–8 (2014).
- Michard, et al., The rise of ward monitoring: opportunities and challenges for critical care specialists. Intensive Care Med; 45(5): 671-673 (2019).
- Michard, et al., Protecting ward patients. ICU Management & Practice; Vol 19 – Issue 1 (2019).
- Semler, et al., Flash mob research: a single-day, multicenter, residentdirected study of respiratory rate. CHEST; 143(6):1740–1744 (2013).
- Sessler, et al., Beyond ‘failure to rescue’: the time has come for continuous ward monitoring. British Journal of Anaesthesia; 122(3): 304-306 (2019).
- Loughlin, et al., Respiratory Rate: The Forgotten Vital Sign – Make It Count! Jt Comm J Qual Patient Saf; 44(8) 494-499 (2018).
- Cretikos, et al., Respiratory rate: the neglected vital sign. MJA; Vol 188 No. 11, 657-659 (2008).
- Keir, et al., The accuracy of respiratory rate assessment by doctors in a London teaching hospital: a cross-sectional study. J Clin Monit Comput; 29:455–460 (2015).
- Taenzer, et al., Postoperative Monitoring—The Dartmouth Experience. The Official Journal of the Anesthesia Patient Safety Foundation; Volume 27, No. 1, 1-28 Circulation 94,429 (2012).
- Brown, et al., Continuous Monitoring in an Inpatient Medical-Surgical Unit: A Controlled Clinical Trial. The American Journal of Medicine; Vol. 127, Issue 3, 226–232.
- Vincent, et al., Improving detection of patient deterioration in the general hospital ward environment. Eur J Anaesthesiol; 35:325-333 (2018).
Ward Monitoring
Paint a future of secure, comprehensive monitoring for the ward