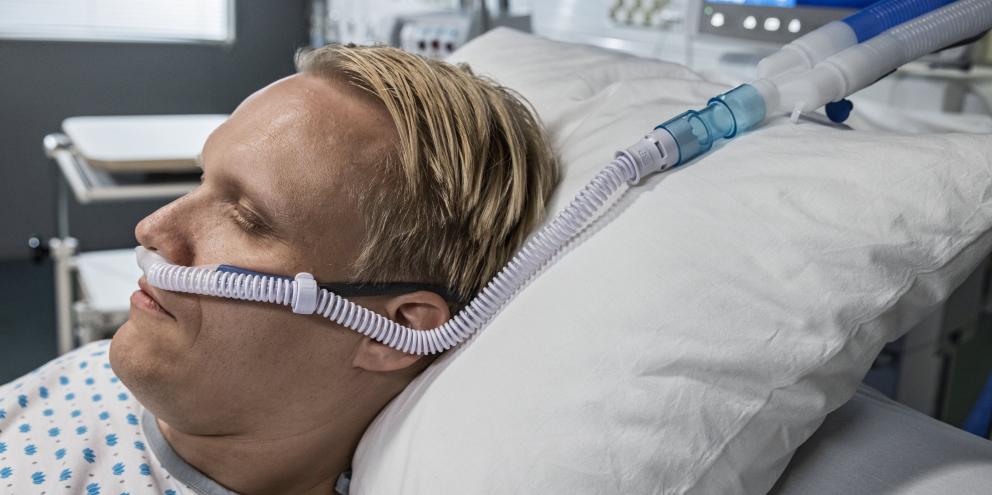
High-flow oxygen therapy (HFOT) is a relatively new modality in oxygen therapy, allowing patients to receive heated, humidified and oxygen-rich gas at a flow exceeding their own inspiratory flow demand1,4. Because of its numerous physiological benefits, including more predictable FiO2 values and reduced work of breathing, it has become a standard of care for pre-oxygenation prior to intubation and post-extubation oxygen support, particularly in the treatment of patients with acute respiratory failure (ARF)4.
During the COVID-19 pandemic, HFOT has offered physician and hospitals a way to care for the patients in the wake of increasing numbers of patients requiring respiratory support2. Because of this, using HFOT has been extended to additional populations, beyond those suffering from ARF. This is particularly true for patients requiring post-extubation oxygen support.
The question is – does HFOT offer benefits over low-flow oxygen therapy for these patients, or does conventional therapy remain superior?
In this article, we’ll answer that question by focusing on the state of current research. We’ll not only look at why HFOT has taken its place in the care of ARF patients, but also delve into the clinical benefits of the modality studies have demonstrated in other patient populations.
Clinical Benefits of HFOT
Physiological benefits that HFOT may offer include4:
- Improved gas exchange and lung mechanics
- Reduced respiratory rate and effort
- Amelioration of dyspnea
- Decreased oxygen dilution
- Decreased anatomical dead-space
- Improved mucociliary function and clearance of secretions
HFOT also possesses a very good safety profile, with possible complications associated with the modality limited to nasal bleeding and mucus dryness, with occasional poor patient tolerance of the device4. Since 2018, 20 randomized controlled trials (RCTs) and 10 meta-analyses have been conducted on HFOT for patients with a variety of clinical conditions1.
We’ll discuss a number of these here.
HFOT compared to Low-flow Oxygen Therapy in ARF
Because of the constant FIO2 that high-flow therapy provides, it has been utilized to treat acute hypoxemic respiratory failure for the past decade. Research has supported this use. Between 2016 and 2018, four meta-analyses found HFOT to be preferrable to conventional therapy for the improvement of oxygenation and avoidance of intubation in patients with hypoxemia1.
Additional research has also been performed with ARF and immunocompromised patients. A meta-analysis by Cortegiani and colleagues comparing low-flow oxygen therapy (LFOT) to HFOT confirmed a reduced risk of intubation with HFOT in this patient population1.
Choosing HFOT over LFOT to reduce intubation rate was also supported by the work of Kang et al1.
HFOT may significantly reduce post-extubation respiratory failure
While conventional LFOT has served as the main supportive treatment after planned extubation, the maximal oxygen flow rates (just 15 L/min) that may be delivered using nasal prongs, cannula or masks is inherently limited3. Unfortunately, this flow rate is insufficient to meet the demands of post-extubation patients with ARF3. Additionally, conventional therapy is also unable to provide for the heating and humidification requirements of these patients3. Because of these potential shortcomings, the mixture of air and oxygen through a heated and humidified circuit and a maximal flow rate of up to 60 L/min, offered by HFOT may better serve these patients, a conclusion supported by Zhu et al3.
Their analysis included 10 studies comparing conventional O2 therapy to HFOT, finding that HFOT may significantly reduce post-extubation respiratory failure and respiratory rates, while increasing PaO2 and is safe to administer after planned extubation3.
Less frequent treatment failure in patients with post-extubation hypoxemia
Theologou et al. delved into the possible benefits of HFOT in cardiac surgery patients with post-extubation hypoxemia, comparing HFOT support with an initial gas flow of 60 or 40 L/min to conventional oxygen therapy4. The researchers determined that the hazard for the primary outcome of treatment failure was lower in patients in both HFOT groups compared to conventional therapy.
Additionally, the probability of peripheral oxygen saturation (SpO2) >92% and respiratory rate within 12–20 breaths/min was 2.4 – 3.9 times higher in an intervention for those receiving support at 60 L/min vs. the other two groups, favoring a higher rate of flow4. The results also showed that in patients receiving HFOT at 40 L/min, desaturation was frequently reversible when gas flow was increased to 60 L/min.
Lower reintubation rates in post-extubation surgical patients
Lu et al. collected and analyzed data from randomized trials and observational studies to assess the benefits of HFOT compared to conventional therapy in post-extubation surgical patients5. While the team found no differences in the incidence of post-operative pulmonary complications (PPCs) or mortality between the two modalities, the results did show that HFOT was associated with a significantly lower reintubation rate and rate of escalation of respiratory support compared with LFOT.
Decreased work of breathing in patients with COPD post-extubation
The choice of HFOT may also benefit patients suffering from chronic obstructive pulmonary disease (COPD) as seen in the work of Di mussi and colleagues6. The researchers compared the effects of HFOT to low-flow therapy on the neuroventilatory drive and work of breathing post-extubation in COPD patients who had received mechanical ventilation for hypercapnic respiratory failure.
They concluded that the use of HFOT following extubation significantly reduced both the neuroventilatory drive and work of breathing compared to conventional therapy.
Significant reduction in need for escalation of respiratory support
Patients undergoing cardio-thoracic surgery are at significant risk of PPCs, with incidence ranging from 8 to 79%7. These PPCs can not only increase length of stay (LOS) in the ICU and hospital, but also morbidity and mortality7. Because of this, anything that can be done to reduce this risk is a vital step to improving patient care and safety.
Wu and colleagues set out to determine whether HFOT could play a role in this PPC risk reduction7. With four studies involving 649 patients, included in the analysis, they determined that compared with low-flow therapy, HFOT was associated with a significant reduction in the escalation of respiratory support and pulmonary complications, although no significant differences in the reintubation rate was found.
Reduced time to recovery and need for mechanical ventilation in COVID-19
At the onset of the COVID-19 pandemic, early observational studies and international guidelines supported the use of HFOT over conventional low-flow therapy in the treatment of patients with severe disease8. However, at the time, the evidence was extremely limited.
Because of this Ospina-Tascón and colleagues set out to compare the effect of HFOT through a nasal cannula on the need for intubation and clinical recovery to conventional therapy in severe COVID-198 cases. Patients in three hospitals in Colombia, who were suffering from respiratory distress and a ratio of partial pressure of arterial oxygen to fraction of inspired oxygen of less than 200 due to COVID-19, were randomly assigned to receive one of the modalities.
The results showed that intubation occurred in 34.3% of patients receiving HFOT compared to 51% on conventional low-flow therapy. Additionally, the median time to clinical recovery within 28 days was 11 days for patients in the HFOT group versus 14 for those randomized to conventional therapy.
Overall, the authors concluded that HFOT served to significantly decrease the need for mechanical ventilation support and time to clinical recovery compared with conventional therapy.
Reduced risk of reintubation and respiratory failure in low-risk patients
While clinical studies have demonstrated the value of HFOT for ARF in critical patients, the benefits observed were at times thought to be attributable to improvements in high-risk patients, raising the question of whether the modality could also benefit low-risk patients9.
That’s why Hernández et al. set out to determine whether HFOT has more benefits compared to conventional therapy for preventing reintubation in mechanically ventilated patients at low risk for reintubation. The researchers conducted a multicenter, randomized clinical trial of 527 patients with planned extubation9.
Once again, the benefits of HFOT were confirmed. Their results showed that:
- Reintubation within 72 hours was less common in the high-flow group (13 patients or 4.9% vs. 32 or 12.2%) in the conventional group
- Post-extubation respiratory failure was also less common with HFOT (22/264 patients or 8.3% vs. 38/263 patients or 14.4%) in the conventional group
The authors concluded that in extubated patients at low risk for reintubation, HFOT reduced the risk of reintubation within 72 hours compared to conventional low-flow therapy.
Conclusion
While HFOT is well-established as the go-to modality for supporting patients with ARF, studies are continuing to confirm the clinical benefits of its use in an expanding number of patient populations. Thus far, research has shown that compared to conventional oxygen therapy, HFOT may reduce the need for re-intubation and the risk of respiratory failure, decrease work of breathing and improve time to recovery. The therapy also improves oxygenation, which is of extreme importance for patients, no matter their disease process.
Sources:
1: Li, Jie et al. “Year in Review 2019: High-Flow Nasal Cannula Oxygen Therapy for Adult Subjects.” Respiratory care vol. 65,4 (2020): 545-557. doi:10.4187/respcare.07663
2: Ashraf-Kashani, N et al. (2017) High-flow nasal oxygen therapy. BJA Education, 17 (2):57–62.
3: Luo, Meng-Si et al. “High-flow nasal cannula oxygen therapy versus conventional oxygen therapy in patients after planned extubation.” Critical care (London, England) vol. 23,1 344. 5 Nov. 2019, doi:10.1186/s13054-019-2606-3
4: Theologou, Stavros et al. “High Flow Oxygen Therapy at Two Initial Flow Settings versus Conventional Oxygen Therapy in Cardiac Surgery Patients with Postextubation Hypoxemia: A Single-Center, Unblinded, Randomized, Controlled Trial.” Journal of clinical medicine vol. 10,10 2079. 12 May. 2021, doi:10.3390/jcm10102079
5: Lu, Zhonghua et al. “Effect of high-flow nasal cannula oxygen therapy compared with conventional oxygen therapy in postoperative patients: a systematic review and meta-analysis.” BMJ open vol. 9,8 e027523. 2 Aug. 2019, doi:10.1136/bmjopen-2018-027523
6: Di mussi et al. “High-flow nasal cannula oxygen therapy decreases postextubation neuroventilatory drive and work of breathing in patients with chronic obstructive pulmonary disease.” Critical Care (2018) 22:180 https://doi.org/10.1186/s13054-018-2107-9
7: Wu, Xiu et al. “Effect of high-flow nasal cannula oxygen therapy vs conventional oxygen therapy on adult postcardiothoracic operation: A meta-analysis.” Medicine vol. 97,41 (2018): e12783. doi:10.1097/MD.0000000000012783
8: Ospina-Tascón, Gustavo A et al. “Effect of High-Flow Oxygen Therapy vs Conventional Oxygen Therapy on Invasive Mechanical Ventilation and Clinical Recovery in Patients With Severe COVID-19: A Randomized Clinical Trial.” JAMA vol. 326,21 (2021): 2161-2171. doi:10.1001/jama.2021.20714
9: Hernández, Gonzalo et al. “Effect of Postextubation High-Flow Nasal Cannula vs Conventional Oxygen Therapy on Reintubation in Low-Risk Patients: A Randomized Clinical Trial.” JAMA vol. 315,13 (2016): 1354-61. doi:10.1001/jama.2016.2711
© 2022 General Electric Company – All rights reserved.
GE and the GE Monogram are trademarks of GE. Reproduction in any form is forbidden without prior written permission from GE. In the United States the O2 Therapy mode used for high-flow oxygen therapy on the CARESCAPE R860 Ventilator is intended to be used for all adult patients and pediatric patients greater than 10 kg in weight. O2 Therapy mode is not available for the neonatal patient type in the United States. Nothing in this material should be used to diagnose or treat any disease or condition. Readers must consult a healthcare professional.
JB22169XX