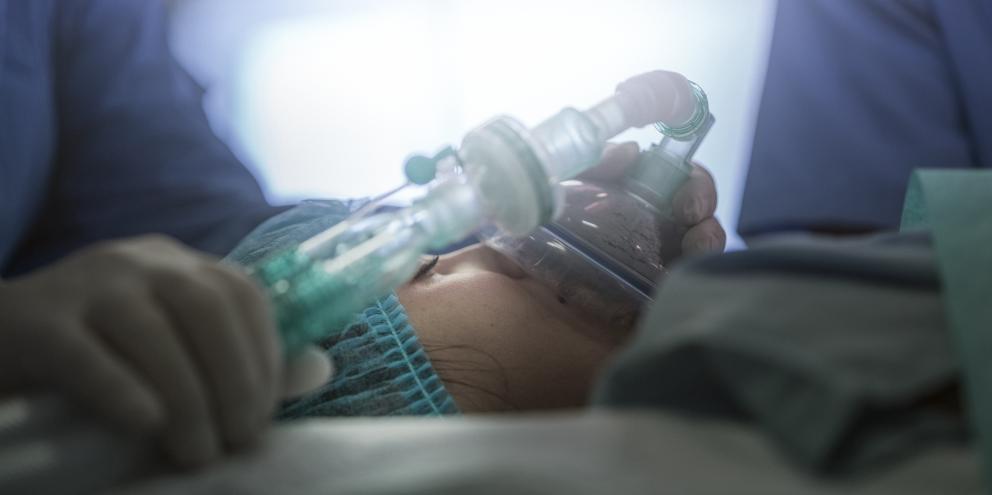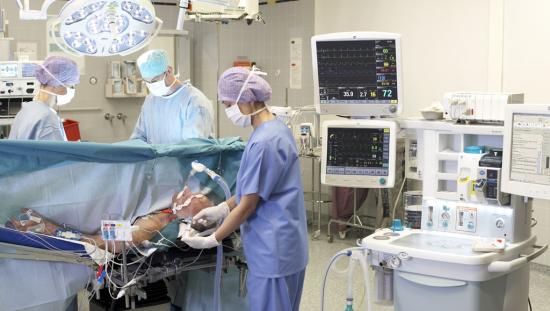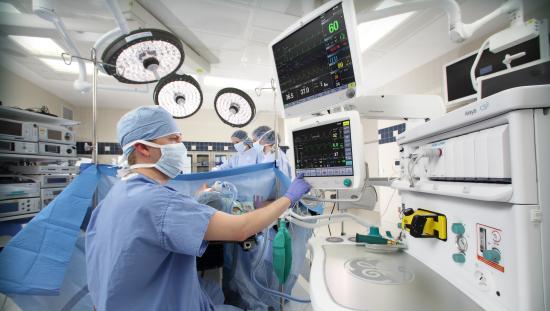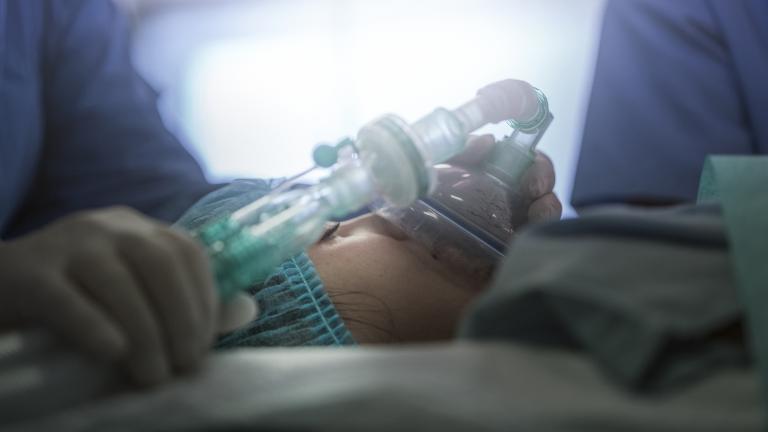
There are many techniques that pediatric anesthesiologists use to anesthetize infants and children. Some use total intravenous anesthesia or TIVA induction, while others use inhalational anesthetics and still others employ a combination of the two. However, regardless of the chosen technique, anesthesia providers must also remember that keeping their "little patients" calm is vital to enhance outcomes in the postoperative phase.
In this article, we’ll discuss the issues that can arise due to perioperative anxiety in children, as well as the most common pediatric induction techniques, including both their benefits and potential downsides. We’ll also dive into the best ways to help an anxious child relax and support a successful induction.
Perioperative anxiety: a common problem
Perioperative anxiety is common for pediatric patients, with studies demonstrating an incidence of anxiolysis of approximately 60%1. There are numerous reasons for these increased feelings of stress, including the fear of being separated from their parents and usual environment, exposure to new people, and equipment that may appear frightening, such as surgical instruments and the anesthetic machine1.
Unfortunately, this anxiety can have a negative impact on the child that lasts beyond the perioperative phase. Anxiety at induction has been associated with a number of adverse clinical outcomes. These may include2:
- Emergence delirium
- Increased analgesic requirements
- Negative postoperative behavioral changes, such as separation anxiety, sleep disturbance, eating problems, aggression and new-onset enuresis
A perioperative experience that results in anxiety may also reduce compliance with future medical procedures necessitated by the child’s condition, including anesthesia2.
Therefore, minimizing distress during anesthesia induction is important for both improving outcomes and reducing the risk of behavioral problems and other issues in the future.
Techniques to consider for anesthesia induction in pediatric patients
Careful consideration must be paid to the choice of technique for induction of anesthesia in infants and children. While many pediatric anesthesiologists have a preferred technique, the age, temperament, individuality and co-morbidities of each individual patient must also be taken into account when choosing between inhalation induction, TIVA or a combination of the two.
Because the majority of children tend to display needle-phobia, inhalation induction is often preferred2. This technique is also the method of choice for children with difficult venous access, as well as a difficult airway, since it supports continuous maintenance of spontaneous ventilation2. In general, inhalation induction is performed using Sevoflurane thanks to its track record as a safe, reliable and quick method to induce anesthesia in pediatric patients2.
However, inhalation induction may also have downsides. First, not all children are calm and easily accept the mask, and the longer the mask is in place, the more a child may protest. Additionally, the volatile gases used may irritate the airway and possess a pungent odor that may increase anxiety in some children. Finally, for children at risk for developing perioperative respiratory complications, research has shown that inhalation induction carries a higher risk than TIVA (26% versus 10.7% incidence of respiratory complications)2. The study authors concluded that children receiving intravenous propofol were significantly less likely to experience perioperative respiratory adverse events compared with those who received inhalational Sevoflurane after adjusting for age, sex, American Society of Anesthesiologists physical status and weight3.
On the other hand, TIVA induction has often been considered more traumatic for pediatric patients due to the need for venous cannulation, which may result in not only pain, but the fear of pain, which should not be discounted. However, this induction technique offers a host of benefits, including rapid induction and the absence of pungent gas to irritate that may irritate the airway. This technique may be most appropriate for a child who already has a venous cannula in situ or those with a high risk of aspiration2.
It is also possible to reduce the risk of pain on cannulation through the use of a topical anesthetic, such as EMLA cream (a mixture of prilocaine and lidocaine)1. It is important to note, however, that the cream must be applied one hour prior to venipuncture to provide effective pain relief and that removing the pain does not necessarily reduce the fear of pain and, therefore, the anxiety of the child1.
Methods to calm little patients and improve outcomes
Because induction carries a risk of anxiety, whether inhalation induction, TIVA or a combination is chosen, calming little patients should be the focus of both anesthesiologists and the nurses who care for these vulnerable patients.
Fortunately, there are a number of techniques that may be utilized to help achieve this goal. However, it is important to consider the age of the child when deciding which is best for the patient, since children react to perioperative stress in an age-dependent manner2. For example, while infants under nine months may separate from parents more easily and experience a smooth inhalation induction through the use of gentle rocking, holding and keeping fasting times to a minimum, between the ages of one and three, anxiety and resistance with any induction method is common2. Therefore, let’s take a look at techniques that should be considered and for which ages they are most appropriate.
Premedication with sedatives
The first option for calming pediatric patients is sedative premedication, which can be used at any age to facilitate smooth separation from the parents and help reduce anxiety during anesthesia induction.
Additional benefits to premedication may include2:
- Decreased risk of aspiration
- Reduced salivation and secretions
- Amnesia, analgesia and anti-emesis
- Reduced total anesthetic requirements
A few of the medications which may be used include2:
- Midazolam – commonly used in children due to its rapid and reliable onset
- Lorazepam and temazempam – useful anxiolytics for older children
- Alpha 2-adrenergic agonists, such as clonidine – used to reduce anxiety in uncooperative children
- Ketamine – can be given as a stun dose intramuscularly for the older, developmentally delayed or autistic child who is uncooperative or combative
- Melatonin – a pineal hormone used to produce natural sleep and reduce the incidence of emergence agitation
Because sedation and respiratory depression may occur with premedication, all patients receiving them must be closely monitored.
Simple explanations and coping mechanisms
For children between the ages of three and 12, explanation and participation is important for anxiety reduction perioperatively, with an increasing need with age2. Because of this, hospital tours, videos, leaflets and interactive books may be helpful. Information should be offered in a manner which is appropriate to their developmental age, and the child should be offered insight into both what will happen on the day of their surgery, and what they will feel. They can also be taught coping mechanisms to help alleviate the stress they feel as the procedure approaches.
Parental presence
There is debate as to whether or not parental presence at induction is useful in reducing anxiety in pediatric surgical patients. While some research has suggested limited benefit, a Cochrane Review of published studies found no benefit of having parents present. Still, some children may benefit from this option, especially in combination with premedication with midazolam, since studies have found a combination of the two is more effective at reducing anxiety in children than parental presence alone1. Children that may benefit from parental presence include those with calm parents, as well as those undergoing repeated procedures2.
Play therapy
Children between the ages of three and six have special concerns, which may include worries regarding bodily mutilation2. For this age group, play therapy may offer help to ease their anxiety. Visual aids, including dolls, videos and interactive books can be employed by a therapist trained in play therapy to reduce negative emotions that affect the induction experience2.
The use of clowns
Clowns have also been used during induction to alleviate anxiety. An Italian study found that children benefitted from the presence of clowns1. However, this presence also resulted in a delay in procedures, as well as interference in the relations between the child and medical personnel1.
Participation
Between the ages of seven and 12 years, participated in their medical care and decision making becomes more important to reducing a child’s anxiety during induction. This can include everything from holding their own mask during induction to choosing a ‘flavor’ for the gas and making ‘mountains’ on the monitor screen with the end tidal CO2 trace1. Adolescents can be involved in the anesthesia plan, allowing them to choose between inhalation and TIVA induction2.
Additional options to reduce anxiety
In addition to the above, methods such as hypnosis, music and lighting can help to create a soothing environment and calm a child in preparation for induction. During the induction itself, distraction may also be useful. This can include the use of toys, blowing bubbles, handling the face mask, playing a video of the child’s choice and more2.
Finally, helping the child become comfortable with breathing through the mask by linking it to a hand-held game may provide improved anxiety relief. Winterberg et al. designed such an interactive interface, by creating a breath-controlled induction app for a tablet, with 3-D animated characters that require the child to breathe into a mask to win mini-games, with the theory that once the child becomes comfortable breathing through the mask pre-operatively, he/she will look forward to completing the next gaming level during induction4.
Summary
As in all aspects of pediatric medicine, anesthesia reduction requires an approach that puts the needs of these little patients at the heart of every choice made. While pediatric anesthesiologists may debate the pros and cons of specific induction techniques, such as inhalation induction and TIVA, no matter which is chosen, special steps must be taken to reduce anxiety, calm fears and enhance outcome for the infants and children in our care.
References
1 : Zielinska, Marzena 3 Holtby, Helen 3 Wolf, Andrew. (2011). Pro-con debate: Intravenous vs inhalation induction of anesthesia in children. Paediatric anaesthesia. 21. 159-68. 10.1111/j.1460-9592.2010.03488.x.
2: Dave, Nandini Malay. Premedication and Induction of Anaesthesia in paediatric patients. Indian Journal of Anaesthesia: September 2019 - Volume 63 - Issue 9 - p 713-720 doi: 10.4103/ija.IJA_491_19.
3: Ramgolam, Anoop et al. “Inhalational versus Intravenous Induction of Anesthesia in Children with a High Risk of Perioperative Respiratory Adverse Events: A Randomized Controlled Trial.” Anesthesiology vol. 128,6 (2018): 1065-1074. doi:10.1097/ALN.0000000000002152
4: Winterberg, Abby V et al. “Optimizing Pediatric Induction Experiences Using Human-centered Design.” Journal of perianesthesia nursing : official journal of the American Society of PeriAnesthesia Nurses vol. 37,1 (2022): 48-52. doi:10.1016/j.jopan.2021.03.001.
© 2023 GE HealthCare.
GE is a trademark of General Electric Company used under trademark license. Reproduction in any form is forbidden without prior written permission from GE. Nothing in this material should be used to diagnose or treat any disease or condition. Readers must consult a healthcare professional.
JB23081XX