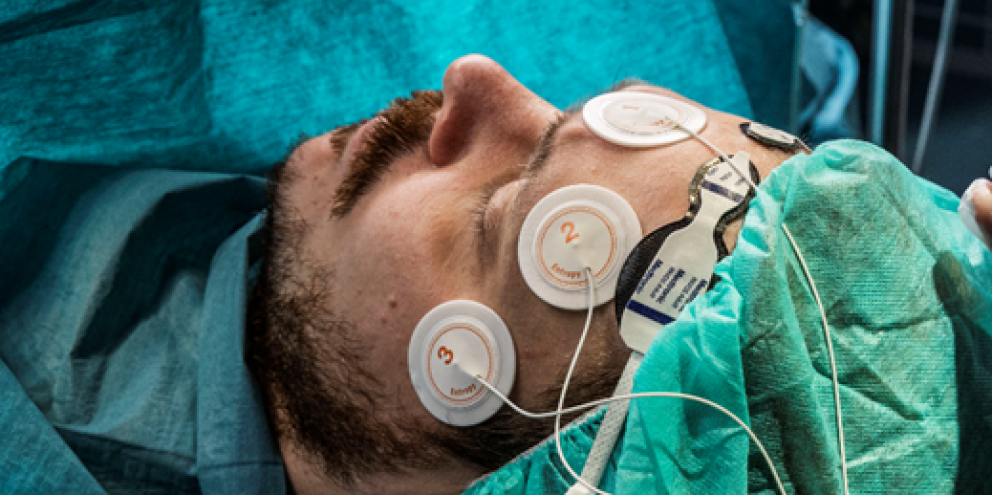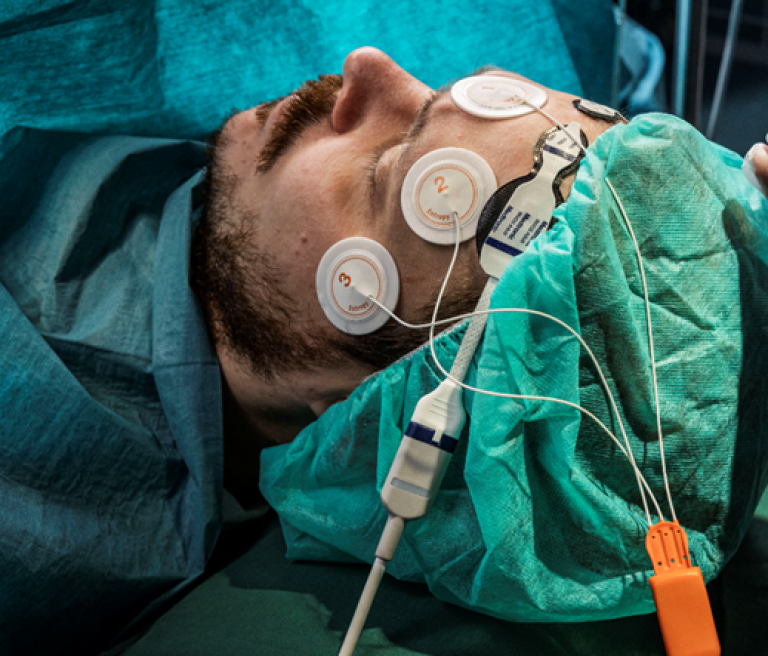
The beach chair position (BCP) has been around since the 1980s and is used frequently when it comes to orthopedic surgeries involving the shoulder. Benefits of BCP include a reduced risk of brachial plexus injury and this access to the shoulder for the surgeon.[1]
However useful, BCP has been shown to increase a patient’s risk for cerebral desaturation. Along with the anesthesia itself, gravity is working against proper perfusion for the patient – especially to the brain. When a patient is placed in a position where they are sitting upright above the horizontal plane, there are expected physiologic responses including decreases in all of the following:1
- Mean Arterial Pressure
- Central Venous Pressure
- Pulmonary Artery Occlusions Pressure
- Stroke Volume
- Cardiac Output
- PaO2
Not only do the above decrease, but there is also an increase in alveolar-arterial oxygen gradient, pulmonary vascular resistance, and total peripheral resistance.1
All of these responses make it more difficult to provide adequate cerebral oxygenation which is made more challenging due to the effects of anesthesia and can lead to cerebral desaturation.
Consequences of cerebral desaturation include stroke, spinal cord ischemia, and visual loss.[2],[3],[4],[5] One way clinicians monitor cerebral perfusion during surgeries involving BCP include measuring blood pressure in both the arm and the leg. This method has proven to be less than ideal and often unreliable when it comes to identifying a cerebral desaturation event.[6]
Due to both the increased risk for cerebral desaturation while using BCP and the severity of consequences of these events, clinicians need a more reliable method of monitoring and detecting changes. One method includes using regional oximetry systems to measure cerebral oxygenation. Regional oximetry allows for real time monitoring and can be used continuously during surgery to detect changes and allow for earlier interventions to improve clinical outcomes.
Beach Chair Position Increases Risk of Cerebral Desaturation Events
There have been multiple studies evaluating the effects on cerebral oxygenation when patients are placed in BCP for orthopedic surgeries. For a patient to have what is considered a cerebral desaturation event (CDE), most researchers quantify this as a 20% or greater relative drop in rSO2 from baseline.
- A small study involving 56 patients undergoing elective shoulder surgery found nearly half (26) of the patients experienced a CDE during the surgery.[7]
- Another small study (n=20) found 80% of patients to have a CDE during shoulder surgery in the BCP.6
- When comparing BCP to the traditional lateral decubitus position (LDP) researchers have explored the differences in rSO2 as well as the difference of variable cerebral oximetry index (COx). When patients had the same shoulder surgery but one group is placed in BCP and the other in LDP, those in BCP had lower rSO2 values and higher COx scores. This difference indicates those in BCP had reduced cerebral autoregulation in addition to lower cerebral oxygen saturation.1
- A review of eight studies involving 1,056 patients undergoing shoulder arthroscopy in the BCP noted the incidence varied quite a bit between studies with CDE incidences ranging from 0% to 57.14%. When averaged, there was an 24.33% incidence of CDEs during surgery all using the parameters of an rSO2 relative decrease of 20% or more from baseline.[8]
BCP and Regional Oximetry
Determining if a patient is going to experience a CDE may be difficult to predict preoperatively. Additionally, blood pressure measurements may not be a reliable method to monitor cerebral perfusion intraoperatively.
Regional oximetry provides timely and accurate information regarding changes in cerebral oxygenation to help detect CDE and intervene quickly.7 With timely identification of CDEs, postoperative complications can be potentially reduced including reducing postoperative cognitive decline in elderly patients undergoing elective orthopedic surgeries.[9]
Regional oximetry has been studied extensively with cardiac surgical patients and has been shown to improve patient outcomes by reducing complications related to CDEs8. While more research is needed to evaluate the specific benefit to orthopedic surgeries where the patient is in BCP, it is clear these patients are at an increased risk of cerebral oxygenation changes due to their surgical position.
With early identification of cerebral oxygenation changes thanks to regional oximetry, clinicians can intervene more quickly to address CDEs and improve clinical outcomes8.
CARESCAPE and INVOSTM
GE HealthCare’s CARESCAPETM monitors software version 3.2 and above are now integrated with regional oximetry capabilities using the CARESCAPE INVOSTM parameter to monitor cerebral oxygenation in the operating room. By using Medtronic’s INVOSTM technology, clinicians are now able to seamlessly monitor regional oximetry in surgical patients, regardless of their surgical positioning.
Cerebral oxygenation is monitored during surgery and captured data follows the patient into the PACU and ICU to provide a more complete picture of patient status to guide clinicians during recovery.
Summary
- Patients undergoing shoulder surgery that involves BCP are at an increased risk of cerebral oxygenation changes
- These changes are difficult to measure using blood pressure readings and difficult to predict preoperatively6
- Regional oximetry allows for real time cerebral oxygenation readings to better identify CDEs and allow for prompt intervention8
- Early identification may lead to improved patient outcomes8
- GE HealthCare’s CARESCAPETM monitors software version 3.2 and above utilize Medtronic’s INVOSTM parameter to seamlessly monitor regional oximetry for clinicians to drive clinical decision making
Disclaimer: The INVOS™ Regional Oximetry Parameter should not be used as the sole basis for diagnosis or therapy and is intended only as an adjunct in patient assessment.
References
[1] Cullen, D & Kirby, R. (2007). Beach chair position may decrease cerebral perfusion. Circulation. 22(2).
[2] Drummond JC, Lee RR, Howell JP Jr. (2012). Focal cerebral ischemia after surgery in the “beach chair” position: the role of a con- genital variation of circle of Willis anatomy. Anesth Analg. 114:1301–3.
[3] Papadonikolakis A, Wiesler ER, Olympio MA, Poehling GG. (2008). Avoiding catastrophic complications of stroke and death related to shoulder surgery in the sitting position. Arthroscopy. 24:481–2
[4] Pohl A, Cullen DJ. (2005) Cerebral ischemia during shoulder surgery in the upright position: a case series. J Clin Anesth. 17:463–9
[5] Bhatti MT, Enneking FK. (2003) Visual loss and ophthalmoplegia after shoulder surgery.(2003) Anesth Analg. 96:899 – 902.
[6] Moerman, A et al. (2012). Cerebral oxygen desaturation during beach chair position. Eur J Anesthesiology. 29(2). 82-7.
[7] Triplet, J et al. (2015). Cerebral desaturation events in the beach chair position: correlation of noninvasive blood pressure and estimated temporal mean arterial pressure. J Shoulder Elbow Surgery. 24(1). 133-7.
[8] Salazar, D. et al. (2019). Cerebral desaturation events during shoulder arthroscopy in the beach chair position. Journal of the AAOS. 3(8). E007.
[9] Yu, Y, Meng, L, & Han, R. (2016). Monitoring cerebral ischemia using cerebral oximetry: pros and cons. J Biomed Research. 30(1). 1-4.