When it comes to environmental sustainability a big question is often ‘how can we make meaningful changes?’. Things like biking instead of driving to work, augmenting energy consumption with solar panels at home, and reducing waste often come to mind.
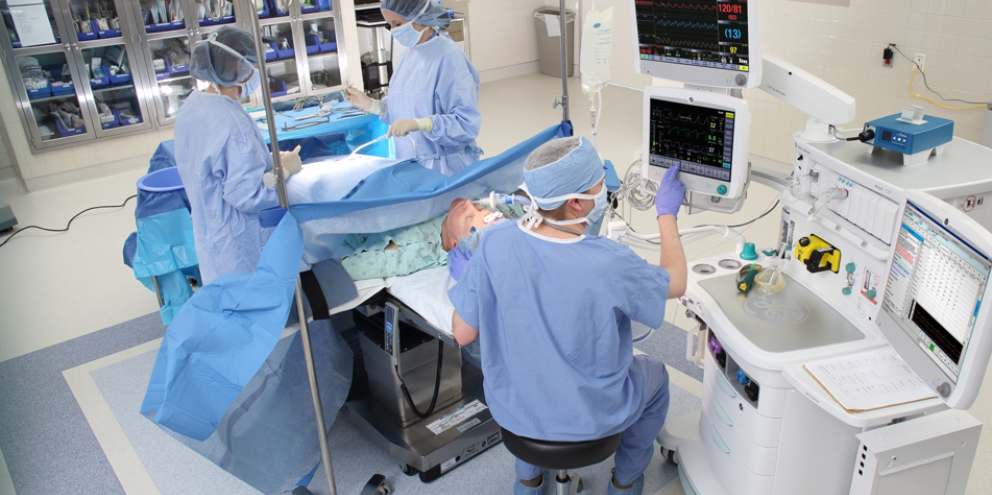
But a major contributor to greenhouse gas emissions has nothing to do with vehicles or remembering to turn the lights off when you leave a room, including the operating room.
Surgical procedures create a large amount of environmental waste thanks to the use of anesthesia gases.[1] These gases can live in the atmosphere for decades and contribute to global warming.
Sevoflurane has a lower impact compared to other gases and has a shorter atmospheric lifespan but there is still room for improvement when it comes to reducing emissions caused by anesthesia procedures.1
The GE HealthCare Sustainability in Anesthesia Webinar Series features three experts from Australia during their second webinar in July 2022 discussing one of these strategies – utilizing low-flow anesthesia. Dr. Alain Kalmar, Dr. Cas Woinarski, and Dr. Ross Kennedy discussed current research surrounding low-flow anesthesia, barriers regarding low-flow practice adoption, and how big data can help address common barriers.
Big data has the potential to provide anesthesiologists with information and motivation to change practice to low-flow anesthesia to not only reduce greenhouse gas emissions, but to reduce overall costs for healthcare systems.
Adoption of Low-Flow Technology Can Save Money and Reduce Ecological Impact
Using sevoflurane instead of desflurane is one way to improve environmental sustainability in the surgical setting1. Sevoflurane has a much lower environmental impact, but still contributes to greenhouse gas emissions.
Dr. Kalmar cites a 1994 article reviewing the specific gravities of various anesthesia gases and notes one 250 ml bottle of sevoflurane is the equivalent of 266 kg of CO2 emissions.[2]
For reference, one bottle of sevoflurane is the equivalent of:
- 111 liters of gasoline
- 2600 km of airline travel
- 1773 km driving
At Maria Middelares General Hospital where Dr. Kalmar practices, sevoflurane consumption was 717 L in 2014. This consumption cost nearly €300,000 and was the equivalent of burning 319,000 L of gasoline.[3] Due to this high level of consumption contributing to greenhouse gases and rising healthcare costs, he studied the impact of using low-flow anesthesia during surgery.
He found when using low-flow anesthesia with end-tidal control software (exclusively to the AisysTM CS2 anesthesia machine) applied with an automated gas control algorithm, consumption could be reduced by more than half during a 40-minute period.3
This reduction could result in annual cost savings of over €5,000-10,000. If sevoflurane is used this could reduce CO2 emissions by 11 tons each year and if desflurane is used the savings would be an astonishing 270 tons annually.3
Using algorithms to facilitate low-flow practices have the potential to help standardize anesthetist practice. Currently, practices vary widely based on location and training. Another way is to use big data to gather data on anesthetist practice.
By doing this, practice patterns can be reviewed with the entire team to identify areas of opportunity. This information can also be reviewed confidentially with individuals to show their own patterns of consumption compared to their colleagues.
Low-Flow Adoption Roadblocks
Dr. Cas Woinarski reviews current roadblocks to low-flow adoption in the surgical setting. He acknowledges there are several levels to changing practices from the highest institutional level to the individual staff behaviors.
A key challenge Dr. Woinarski notes is the current fresh gas flow recommendation in the written sevoflurane product information. The sevoflurane product instructions currently state fresh gas flow rates below 2L/min in a circle absorber system are not recommended due to “limited clinical studies” and the concern for Compound A production.[4]
However, Dr. Woinarski cites the 2019 article published in Anesthesia and Intensive Care which reports that low-flow practices do not pose a risk for Compound A production. Additionally, Compound A is a product shown to be toxic in rats but not in humans.[5]
Although low-flow rates have been shown to be safe, the manufacturer's statement makes using sevoflurane in a low-flow state an off-label use for clinicians and could deter using the anesthesia gas in the more environmentally stable setting.
Another barrier Dr. Woinarski points out is the assumption using low-flow anesthesia increases the absorbent cost to a point that any cost savings are negated. Feldman et al. is cited to counter this assumption by noting absorbent costs are still reduced when using low-flow sevoflurane in a closed system.[6]
Adopting new technologies, especially ones that include automation may be a barrier to some anesthetists. More research is being done to show how automation can increase the use of low gas flows while lowering costs. Dr. Woinarski cites a 2013 article reviewing the EtControlTM software and gas module on the GE HealthCare Aisys CS2 Anesthesia machine.[7]
Researchers evaluated fresh gas flow for 321 patients comparing the use of the automated fresh gas control versus manual control. The average desflurane consumption using the automated model was 27 ml h-1 while the manual control model was much higher at 45 ml h-1.7
Another study evaluating the Aisys anesthesia machine (as well as the Flow-i® machine) found using automated gas delivery systems reduced consumption from 25.8 to 15.2 ml during a 60 minute period.[8]
Adopting low-flow practices can help reduce anesthesia gas emissions but change is often slow in healthcare. Using big data to gather information and use it to support clinician change can potentially hasten the rate of low-flow practices.
Summary
- Big data helps gather proof of opportunities to reduce carbon footprint and save money
- Benchmarking individuals may help incentivize clinicians and illustrate the feasibility of adopting a new practice
- Low-flow anesthesia is safe and economical
- Using an automated fresh gas flow anesthesia delivery system has the potential to promote adoption of low-flow practices in the operating room
© 2022 General Electric Company – All rights reserved.
GE and the GE Monogram are trademarks of GE. Flow-i® is a registered trademark of Maquet Critical Care AB Ltd. Reproduction in any form is forbidden without prior written permission from GE. Nothing in this material should be used to diagnose or treat any disease or condition. Readers must consult a healthcare professional.
End-tidal control is not available in all markets. In the USA, Et Control is indicated for patients 18 years of age and older.
JB22663XX
References
[1] GE HealthCare Clinical View. (2022). Practical ways to reduce the environmental impact of anesthesia. Accessed Oct 10, 2022. https://clinicalview.gehealthcare.com/article/practical-ways-reduce-environmental-impact-anesthesia#_ftnref1
[2] Laster, M, Fang, Z, & Eger, E. (1994). Specific gravities of desflurane, enflurane, halothane, isoflurane, and sevoflurane. Anesthesia & Analgesia. 78(6):1152-3.
[3] Kalmar, A et al. (2022). Minimizing sevoflurane wastage by sensible use of automated gas control technology in the flow-I workstation: an economic and ecological assessment. Journal of Clinical Monitoring and Computing.
[4] FDA. (2003). ULTANE (sevoflurane) volatile liquid for inhalation. Accessed Oct 10, 2022. https://www.accessdata.fda.gov/drugsatfda_docs/label/2006/020478s016lbl.pdf
[5] Kennedy, R et al. (2019). There are no dragons: low-flow anesthesia with sevoflurane is safe. Anesthesia and Intensive Care. 47(3).
[6] Feldman, J, Lo, C, & Jan, H. (2020). Estimating the impact of carbon dioxide absorbent performance differences on absorbent cost during low-flow anesthesia. Anesthesia & Analgesia. 130(2): 374-381.
[7] Singaraelu, S & Barclay, P. (2013). Automated control of end-tidal inhalation anesthetic concentration using the GE Aisys Carestation. British Journal of Anasthesia. 110(4):561-566.
[8] Mostad, D, Klepstad, P, Follestad, T, & Pleym, H. (2021). Desflurane consumption with automated vapour control systems in two different anesthesia machines. A randomized controlled study. Anaesthesiologica Scandinavica. 65(7):895-901.