As an oxygen transporter, hemoglobin is a vital red blood cell protein for hemodynamic stability.
There are several reasons why hemoglobin values may drop, such as internal bleeding, acute or chronic illnesses, or procedures including surgery.[1] When hemoglobin values drop, patients may need a transfusion of packed red blood cells to replace hemoglobin or fluid administration to maintain appropriate hemodynamic status.
While standard pulse oximetry remains a useful tool in monitoring oxygenation status, it only measures the percentage of oxygenated hemoglobin in the blood rather than measuring the hemoglobin value. Clinicians measure hemoglobin along with other patient factors to determine the need to transfuse.[2]
Unfortunately, traditional methods of hemoglobin monitoring may provide values intermittently. This is due to the multiple steps required to obtain the lab values.
First, the blood sample must be collected from a venous puncture and then transported to the laboratory where it waits for analysis. Once the blood has been analyzed, the results must be uploaded to the patient chart and only then can the clinician review the results.2
These lab results are intermittent spot checks, providing a singular value from a point in time.
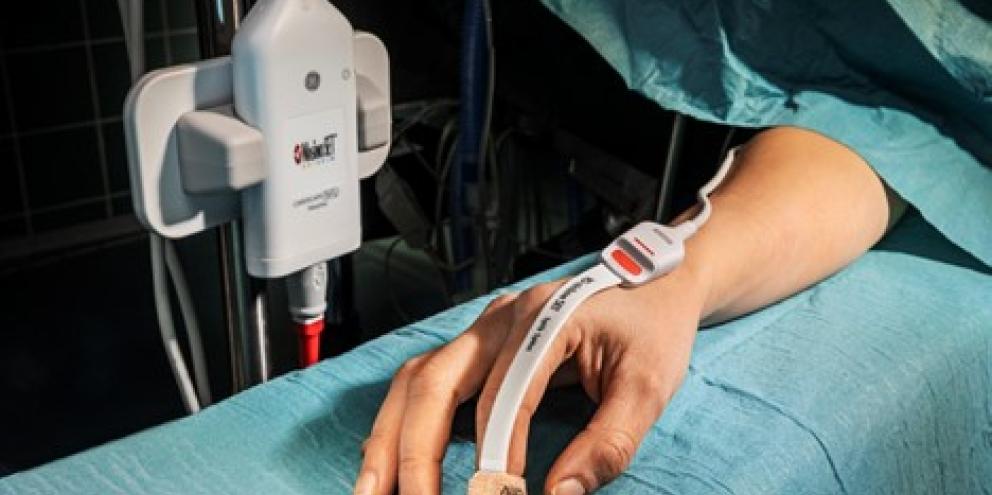
Masimo rainbow SET® Pulse CO-Oximetry provides a unique method of hemoglobin monitoring – one that is continuous and noninvasive. In addition to hemoglobin readings using SpHb®, Masimo rainbow SET® sensors provide pulse oximetry measurements, oxygen saturation (SpO2), pulse rate (PR), perfusion index (Pi), and pleth variability index (PVi®).
This article will describe some of the benefits of monitoring these parameters with the Masimo solution including the evidence showing reduction in unnecessary transfusions and improvement in patient outcomes.
Benefits of Continuous Hemoglobin Monitoring
While transfusions can help improve patients’ hemoglobin status, analysis of several studies have shown that many transfusions are administered inappropriately3 and without actual benefits to the patient. Unnecessary blood transfusions are costly4 and can contribute to an increase in morbidity and mortality.5 Decreasing hemoglobin values are often a key sign that a transfusion is required to address blood loss. Real-time, continuous monitoring provides clinicians with more visibility to patients’ hemoglobin.
This can be important because where there is a delay in blood loss detection and the subsequent needed intervention, the risk for adverse patient outcomes increases.6
Using continuous hemoglobin monitoring has been recommended to help blood management by providing real-time trends visible on the patient’s monitor at the bedside.7 This can be done using SpHb, which shows the trend of hemoglobin concentration in arterial blood using multi-wavelength technology.
Continuous SpHb readings provide a more complete picture of a patient’s hemoglobin changes than intermittent hemoglobin values and have been shown in multiple studies to help improve blood management.
Please visit this page for references associated with outcomes
When looking at patient benefits in a surgical setting, a 2016 study found continuous hemoglobin monitoring using SpHb:8
- Helped decrease the percentage of patients needing transfusion by 7.4%
- Helped decrease the total number of transfused units per patient by 12.56%
- Allowed for cost savings of €20.59 per patient
Perfusion Index and Pleth Variability Index
Perfusion Index (Pi) is the ratio between the constant and variable amounts of light absorbed by arterial blood flow in the skin. Simply put, it is the ratio of pulsing to non-pulsing blood.
A lower value indicates lower perfusion.
Relative changes in peripheral perfusion status can be monitored non-invasively and continuously using Pi from the Masimo pulse oximeter. A site with a higher Pi number generally helps to improve the monitoring confidence for pulse oximetry and Pulse CO-Oximetry measures.
The response to patient interventions can be tough to track with static measurements. Therefore, the trending data tends to be more useful and informative.
The Pleth Variability Index (PVi®) is an index that may be used as a non-invasive, dynamic indicator of fluid responsiveness in select populations of mechanically ventilated adult patients from a single pulse oximetry sensor.9 This index is derived non-invasively through pulse oximetry and can therefore be used even when a patient does not have an arterial line.
Research has illustrated the usefulness of monitoring PVi as a fluid responsiveness indicator in both the operating room and intensive care units.10,11
PVi monitoring during a clinical trial of surgical patients has been found to support enhanced recovery as well as improved patient satisfaction and significant reductions in:12
- Length of hospital stay
- Complication rates
- Patient costs
For example, a study of over 18,000 patients found when SpHb and PVi are monitored together using the hospital’s goal-directed protocol, there was a significant reduction in post-surgical mortality at both 30- and 90-days post-op.13
Optimal patient management involves accurate and timely monitoring of various patient status indicators. Being able to monitor SpHb, Pi, and PVi together in real-time technology provides meaningful trended data that can support clinical decision-making to help improve patient outcomes.
Summary
- Monitoring hemoglobin using traditional methods alone may result in delayed and static information 2
- Continuous hemoglobin monitoring using SpHb provides insight into hemoglobin between invasive samples and has been shown to improve blood transfusion management 7, 8
- Pi and PVi can change with fluid levels and can provide additional continuous data to support clinician decisions, especially in the operating room and intensive care unit with certain populations of intubated and mechanically ventilated patients 10,11, 12
- Masimo rainbow SET® Pulse CO-Oximetry provides all three of these measurements among other clinical parameters, providing real-time information using a non-invasive monitoring solution
References
[1] World Health Organization. 2008. Global Database on Anemia.
2 Miller, R.D. (2015) Miller’s Anesthesia. 8th Edition.
3 Shander et al. TransMed Rev. 2011. 232-246
4 Shander et al. Transfusion. 2010;50(4):753-765
5 Marik, P & Corwin, H. (2008). Efficacy of red blood cell transfusion in the critically ill: a systematic review of the literature. Crit Care Med. 36(9):2667-74.
6 Herwaldt LA. (2003). Hemorrhage after coronary artery bypass graft procedures. Infect Control Hosp Epidemiol. 2003; 24(1):44-50
7 Society for the Advancement of Blood Management (SABM). Improvement of Patient Outcomes with Hemoglobin Monitoring in the Critical Care and Perioperative Setting. Publications. 2021, January. https://sabm.org/wp-content/uploads/SABM-HbMonitoringWhitepaper.pdf
8 Ribed-Sanchez, B et al. (2018). Economic analysis of the reduction of blood transfusions during surgical procedures while continuous hemoglobin monitoring is used. Sensors (Basel). Apr 27;18(5):1367.
9 Accuracy of PVi in predicting fluid responsiveness is variable and influenced by numerous patient, procedure and device related factors. PVi measures the variation in the plethysmography amplitude but does not provide measurements of stroke volume or cardiac output. Fluid management decisions should be based on a complete
assessment of the patient’s condition and should not be based solely on PVi.
10 Zimmermann, M et al. (2010). Accuracy of stroke volume variation compared with Pleth variability index to predict fluid responsiveness in mechanically ventilated patients undergoing major surgery. Eur J Anesthesiology. 27(6):555-61.
11 Loupec, T. (2011). Pleth variability index predicts fluid responsiveness in critically ill patients. Crit Care Med. 39(2):294-9.
12 Thiele, R et al. (2015). Standardization of care: impact of an enhanced recovery protocol on length of stay, complications, and direct costs after colorectal surgery. J Am Coll Surg. 220(4):430-43.
13 Cros, J et al. (2019). Continuous hemoglobin and plethysmography variability index monitoring can modify transfusion practice and is associated with lower mortality. J Clin Monit Comput. 34(4):683-691.