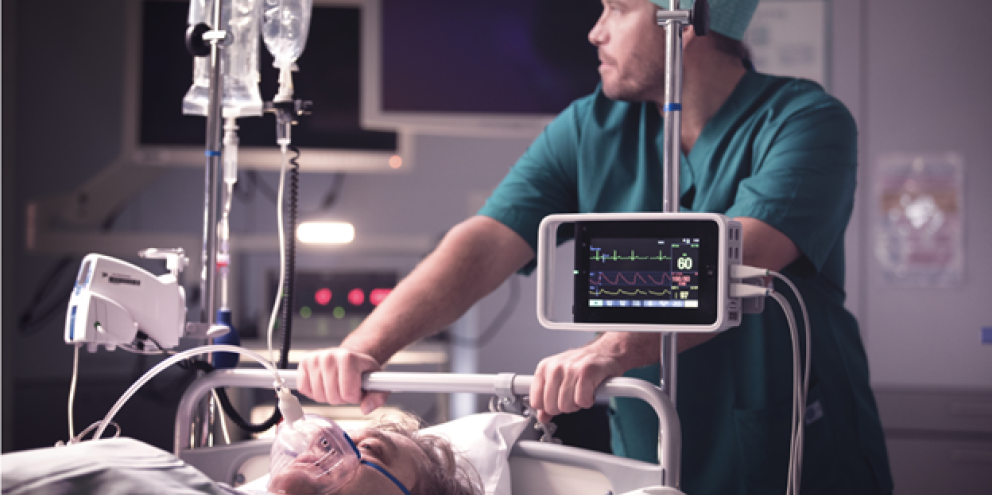
Maintaining an optimal fluid status in surgical and critical care patients plays a vital role in patient outcomes. Too little fluid and you risk decreased tissue and organ perfusion and excessive fluid can add additional stress to the heart.
In critically ill patients who are mechanically ventilated, there is an expected change in blood pressures. This includes blood flow to the vena cava, pulmonary artery, and aorta.[1]
Research has shown the extent of these changes, or arterial pressure variations, depends greatly on the patient’s volume status.1
Pressure variations, rather than static pressure measurements, can help predict a patient’s fluid responsiveness. This indicator can provide clinicians vital information and drive clinical decision making when it comes to supporting patients and their fluid volume needs.1
Today there are devices available to monitor pulse pressure variation (PPV) and systolic pressure variation (SPV) that are minimally invasive, using the data already being collected from traditional arterial lines. These devices are also able to create trends and detect subtle variations while saving clinicians time from doing frequent manual calculations.
This article covers a few of the main benefits of PPV/SPV monitoring devices and their application in the critical care setting.
Monitoring Fluid Status is Vital
Managing surgical or critically ill patient fluid volume is complex due to several factors. Anesthesia inherently reduces fluid volume and blood pressure and decreases tissue perfusion during surgery.[2] And although current protocols are shifting away from strict fasting prior to surgery, many patients enter the surgical suite dehydrated at a baseline.2
Pumping patients up with fluids to mitigate volume loss leads to additional problems including volume overload. This can strain the heart, cause pulmonary edema, prolong wound healing, and even impact bowel function.[3] Additional problems arise with volume overload, leading clinicians to turn to various fluid status assessment tools to drive decision making.2
Although complicated, optimizing peri-operative fluid status (especially in high-risk patients) has been shown to improve post-operative outcomes.[4]
Ways to Monitor Fluid Volume Status
Historically, measuring central venous pressure or pulmonary capillary wedge pressure have been used to assess patient fluid volume. However useful, these static measurements are invasive limiting their practicality and do not provide much predictive power when it comes to determining if a patient will respond to fluid therapy.2
Monitoring arterial pressure variation and identifying trends in data rather than static pressure measurements can provide more value, especially when it comes to predicting outcomes.
Arterial pressure variation is calculated by measuring SPV or PPV variations.2 SPV is calculated with the following equation:1
SPV [mmHg]= SBPmax - SBPmin
PPV is calculated with a slightly more complex equation:1
PPV [%]= (PPmax - PPmin) / [(PPmax + PPmin) / 2] * 100
The changes, or delta, in systolic arterial pressures help predict if a patient will respond to fluid therapy or not. Measurements are collected right before lung inflation after a respiratory pause, in order to complete the equation.
Research shows there are certain ranges of percentages that can serve as cues of fluid responsiveness.[5] If a percentage is between 10-15%, this may be a strong indication for fluid responsiveness while 8-12% is generally considered a grey area and requires additional insights to make a treatment decision.5
This measurement can drive clinical decision making regarding administering fluids or using medications supporting vascular resistance or cardiac function.
Benefits of Using SPV / PPV Devices
Clinicians can manually calculate these variations, but these calculations take time to complete as well as time to analyze and evaluate trends. This has led to parameters such as PPV and SPV being readily available in many patient monitoring devices.
When PPV/SPV monitoring guides clinical decision making, it has been shown to improve patient outcomes. Outcomes including reduced post-surgical morbidity and reduced length of stay in the ICU.1
PPV/SPV monitoring can be done with a minimally invasive arterial line, including radial artery catheterization, and does not require pulmonary artery catheterization. While useful to monitor pulmonary hypertension and estimate cardiac output, pulmonary artery measurements alone do not provide much insight into predicting if a patient will respond to fluid therapy.[6]
Pulmonary artery catheterization also carries a new set of risks. The catheter can migrate leading to arrhythmias, valve rupture, or cardiac wall perforation.5 Due to these additional risks as well as little perceived predictive value, using PPV/SPV monitoring is becoming more appealing to clinicians.
Not only are PPV/SPV measurements less invasive and reduce workload for clinicians, but studies have also shown their superiority to static metric of cardiac preload when it comes to predicating fluid responsiveness.[7]
Summary
- Fluid status changes are expected and should be anticipated in surgical and critically ill patients
- Monitoring pressure variations can provide more fluid status predictive power than static pressure measurements
- SPV/PPV calculations can help guide clinical decision-making surrounding fluid responsiveness
- SPV/PPV devices can help save clinicians time and help them improve patient outcomes
References
[1] Michard, F. (2005). Changes in arterial pressure during mechanical ventilation. Anesthesiology. 103. 419-428.
[2] Rathore, A et al. (2017). Validity of pulse pressure variation (PPV) compared with stroke volume variation (SVV) in predicting fluid responsiveness. Turkish Journal of Anesthesiology and Reanimation. 45(4): 210-217.
[3] Rolando, C & Mehta, R. (2016). Fluid overload in the ICU: evaluation and management. BMC Nephrology. 17 (109).
[4] Willars, C, Dada, A, Hughes, T, & Green, D. (2012). Functional hemodynamic monitoring: the value of SSV as measured by the LiDCORapid in predicting fluid responsiveness in high risk vascular surgical patients. Int J Surg. 10(3):148-52.
[5] Deflandre, E, Bonhomme, V, & Hans, P. (2008). Delta down compared with delta pulse pressure as an indicator of volaemia during intracranial surgery. Biritish Journal of Anesthesia. 100(2): 245-250.
[6] Ziccardi, M. & Khalid, Nauman. (2021). Pulmonary artery catheterization. NCBI StatPearls.
[7] Preisman, S, Kogan, S, Berkenstadt, H, & Perel, A. (2005). Predicating fluid responsiveness in patients undergoing cardiac surgery: functional haemodynamic parameters including the respiratory systolic variation test and static preload indicators. British Journal of Anaesthesia. 95(6): 746-755.